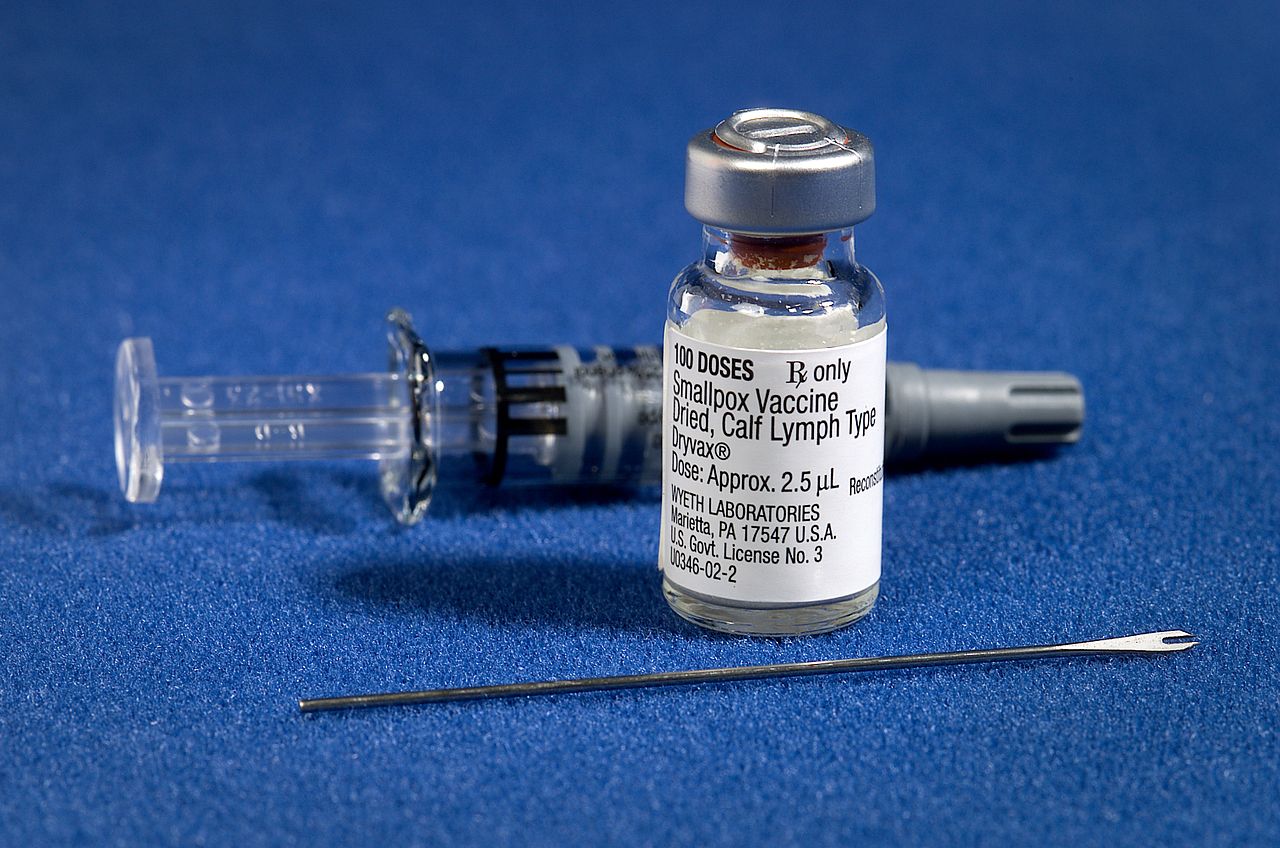
The Unprecedented Triumph: Eradicating a Global Scourge with the Smallpox Vaccine
Smallpox was once one of humanity's most feared and devastating diseases, claiming millions of lives over centuries and leaving survivors often disfigured or blind. Its relentless spread across continents brought untold suffering, leaving no community untouched. Yet, this ancient scourge met its match in one of the greatest scientific achievements in history: the development and global deployment of the
Smallpox Vaccine. It stands as a singular testament to medical innovation, a shot that literally changed the course of human health by eradicating an entire disease.
The story of the smallpox vaccine is inextricably linked to the pioneering work of British physician Edward Jenner. In 1796, Jenner observed that milkmaids who had contracted cowpox, a milder disease, seemed immune to smallpox. This crucial insight led him to inoculate a young boy with material from cowpox lesions, demonstrating that this exposure conferred protection against the deadly variola virus responsible for smallpox. Jenner famously referred to cowpox as *variolae vaccinae* (smallpox of the cow), from which the very term "vaccine" (derived from *vacca*, the Latin word for cow) originates. His discovery laid the foundational stone for modern immunology and public health.
While Jenner's method utilized the cowpox virus, the modern smallpox vaccine, which emerged later in the 20th century, primarily employed the vaccinia virus. This related but distinct orthopoxvirus proved highly effective in providing cross-protection against smallpox. Building on this scientific breakthrough, the World Health Organization (WHO) launched an ambitious global vaccination campaign from 1958 to 1977. This monumental effort involved coordinated mass vaccination, surveillance, and containment strategies across the globe. The campaign's success was absolute: in 1980, the WHO officially declared smallpox eradicated, making it the only human infectious disease ever to be completely wiped out from the face of the Earth. This achievement remains a beacon of what is possible through dedicated global cooperation in public health.
How the Smallpox Vaccine Works: A Scientific Marvel
The effectiveness of the smallpox vaccine lies in its ingenious use of the vaccinia virus. Unlike some vaccines that use weakened forms of the disease-causing pathogen, the smallpox vaccine utilizes vaccinia – a virus that is genetically distinct from variola (smallpox) and cowpox, but shares enough antigenic similarities to stimulate a robust immune response that protects against smallpox. This phenomenon is known as *cross-protection*. When introduced into the body, the vaccinia virus safely prompts the immune system to produce antibodies and T-cells capable of recognizing and neutralizing the variola virus if exposed later.
Administering the traditional smallpox vaccine was a unique process, a far cry from the single intramuscular shot common today. It typically involved a specialized instrument called a *bifurcated needle*. This small, two-pronged needle was dipped into the vaccine solution and then used to rapidly puncture the skin surface multiple times. For a primary vaccination, typically three punctures were made, while revaccination might involve up to fifteen. These punctures were performed with enough vigor to ensure a trace of blood appeared within 15 to 20 seconds, indicating that the vaccine had successfully entered the superficial layers of the skin. Proper administration was crucial for its near 100% effectiveness.
The site of vaccination usually did not require extensive preparation, though if alcohol was used for cleaning, it was imperative to allow the skin to dry completely to prevent inactivation of the live virus in the vaccine. Following a successful primary vaccination, known as a "primary take," a characteristic progression of reactions would occur. Within three to four days, the vaccination site would typically become reddened and itchy (pruritic). By seven to eleven days, a prominent, fluid-filled vesicle surrounded by a red ring (areola) would form, eventually becoming pustular. This lesion would then scab over by the third week, leaving a distinctive scar that served as visible proof of successful immunization. This unique reaction pattern confirmed the body's immune system was responding effectively.
Navigating the Risks: Why Routine Vaccination Stopped
While the smallpox vaccine was an undeniable triumph in disease eradication, its widespread use was not without significant drawbacks concerning safety. The very nature of a live virus vaccine, even one using a relatively benign orthopoxvirus like vaccinia, meant that adverse reactions were more common and potentially more severe than those associated with many modern vaccines. The most frequent side effect was fever, a generalized response as the body mounted an immune defense. However, more serious complications, though rare, posed substantial risks.
Among the most concerning adverse events were:
- Eczema Vaccinatum: A severe, sometimes fatal, generalized vaccinia infection that occurred in individuals with a history of eczema, atopic dermatitis, or other exfoliative skin conditions. The virus could spread rapidly across compromised skin, leading to extensive lesions.
- Vaccinia Necrosum (Progressive Vaccinia): A severe, progressive destruction of tissue at the vaccination site and potentially elsewhere, primarily observed in immunocompromised individuals. Their weakened immune systems were unable to contain the vaccinia virus, leading to uncontrolled replication.
- Autoinoculation: The accidental transfer of the vaccinia virus from the vaccination site to other parts of the body, most commonly the eyes. This could cause painful keratitis and, in severe cases, permanent scarring and vision impairment.
- Generalized Vaccinia: A widespread rash of vaccinia lesions across the body, typically a benign but unsettling complication.
- Myopericarditis and Encephalitis: Inflammation of the heart muscle/sac or the brain, respectively. These were rare but potentially life-threatening complications.
Statistical data highlighted these risks: it was estimated that 14 to 52 out of every million primary vaccinees experienced serious or life-threatening adverse reactions. The risk of death from vaccinia was approximately one case per million primary vaccinations. These figures, while seemingly low, became unacceptable once the threat of naturally circulating smallpox was eliminated.
Furthermore, the live attenuated vaccinia virus vaccine had extensive contraindications, effectively making it unsuitable for a significant portion of the population – up to 30% or more. These included:
- Infants
- Pregnant women and women who were breastfeeding
- Immunocompromised individuals (e.g., those with HIV/AIDS, cancer patients undergoing chemotherapy, organ transplant recipients)
- People with eczema or other exfoliative skin disorders
- Individuals living in the same household or having intimate contact with anyone in the above high-risk groups, due to the risk of secondary transmission via autoinoculation.
- People with certain cardiovascular conditions.
Given these substantial safety limitations and the eradication of smallpox, routine vaccination of the general public was rightly discontinued. The risks simply far outweighed the benefits in a world free of the variola virus. For a deeper dive into who should avoid the vaccine, you can read our detailed article on
Smallpox Vaccine Risks: Who Should Not Get Immunized?.
Modern Relevancy: Beyond Eradication
Despite its eradication, the story of the smallpox vaccine did not end in 1980. The potential for the variola virus to be weaponized as a tool of bioterrorism or biological warfare has ensured that the vaccine remains a critical asset in national and global health security strategies. Although stockpiles of the virus are officially confined to highly secure laboratories, the specter of its deliberate release necessitates preparedness.
Beyond the threat of smallpox itself, the vaccine has found renewed relevance in protecting against other related orthopoxviruses, most notably mpox (formerly monkeypox). Mpox, which has recently garnered global attention, is caused by a virus genetically similar to variola. The smallpox vaccine has shown significant efficacy in preventing mpox infection and mitigating disease severity, making it a crucial tool in managing outbreaks of this emerging threat.
Concerns over the safety profile of traditional live vaccinia virus vaccines, particularly the calf-lymph-derived versions, have spurred the development of alternative smallpox vaccines. These newer generations aim to maintain efficacy while significantly reducing adverse events, especially for civilian populations who might lack natural immunity and present a broader range of health conditions. For instance, new vaccines derived from cell cultures have been developed and rigorously tested. One such cell-cultured vaccine, compared with a traditional calf-lymph-derived vaccine in studies involving healthy adults, demonstrated comparable immunogenicity (ability to provoke an immune response) and safety. While both groups experienced similar adverse reactions (such as localized "pock lesions"), the move towards cell-cultured vaccines offers a safer and more scalable production method, crucial for potential widespread deployment without the severe limitations of older versions. This evolution ensures that humanity maintains a robust defense, ready to respond to unforeseen threats. To explore this further, delve into
Beyond Eradication: The Smallpox Vaccine's New Role.
Conclusion
The smallpox vaccine holds an unparalleled place in medical history. It stands as the first vaccine against a contagious disease and the only tool responsible for the complete eradication of a human pathogen. From Edward Jenner's serendipitous observations to the WHO's monumental global campaign, its legacy is one of triumph over immense suffering. While the inherent risks of traditional vaccinia-based vaccines led to the cessation of routine immunization, its importance has never truly faded. In a world grappling with bioterrorism concerns and emerging viral threats like mpox, the smallpox vaccine, in its traditional and newer, safer forms, continues to be a vital component of our public health arsenal, reminding us of both the power of scientific innovation and the enduring need for vigilance.